blog spot
THE
health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
CATEGORY
4/06/2026
POSTED
As the weather warms up in Northern Virginia, families are spending more time outdoors — at parks, trails, sports fields, and even in their own backyards. But with that increase in outdoor activity comes a higher risk of tick bites and Lyme disease.
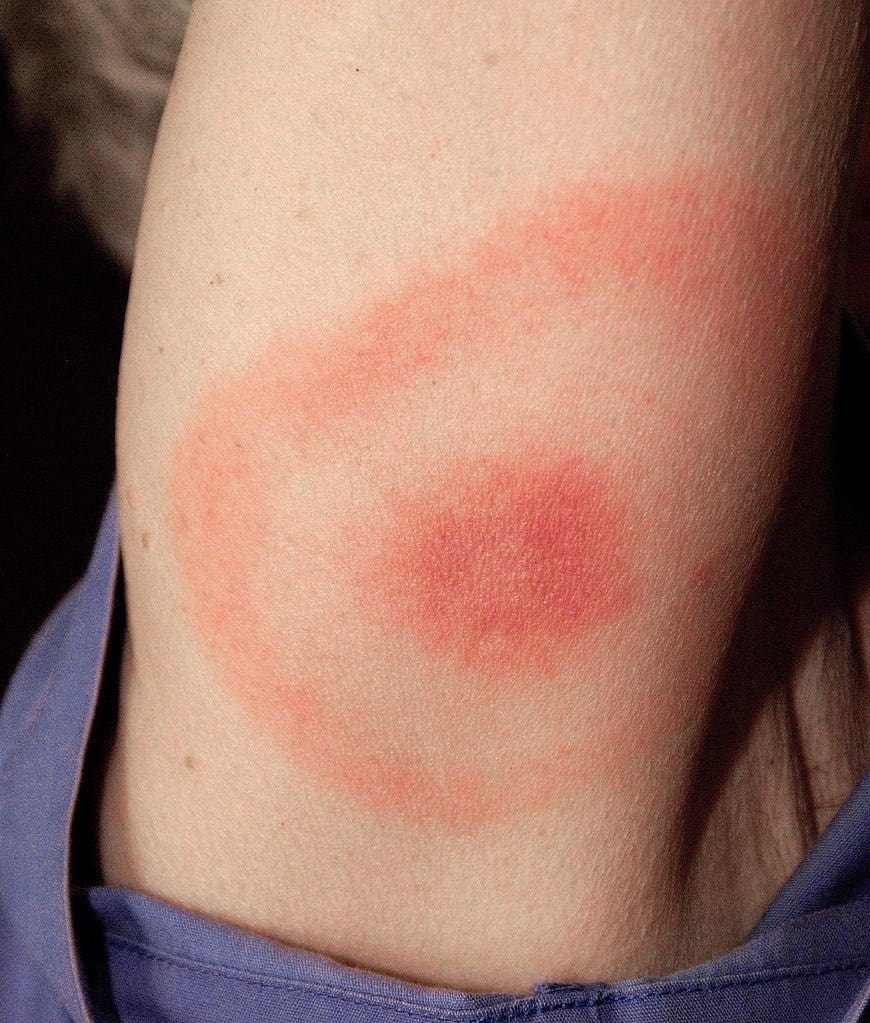
According to a recent Loudoun County health update, tick season is highest from May through October, and our area continues to report some of the highest Lyme disease rates in Northern Virginia.
Understanding how to prevent tick bites — and recognizing early symptoms — can help protect your family during the months ahead.
What Is Lyme Disease?
Lyme disease is a bacterial infection spread through the bite of an infected blacklegged tick (also known as a deer tick).
These ticks are commonly found in wooded areas, tall grass, and brush, making everyday outdoor activities a potential source of exposure.
Lyme disease is the most common tick-borne illness in Loudoun County, but other tick-related illnesses can also occur, which is why awareness is important.
Signs and Symptoms of Lyme Disease
One of the challenges with Lyme disease is that symptoms don’t always appear right away — and many people don’t remember being bitten by a tick.
Early symptoms may include:
- Fever or chills
- Fatigue
- Headaches
- Muscle or joint pain
- A “bull’s-eye” rash (erythema migrans)
These symptoms can feel similar to a viral illness, which is why they’re sometimes overlooked.
If untreated, Lyme disease can affect the joints, heart, and nervous system, making early recognition and treatment especially important.
When Does Lyme Disease Spread?
Ticks can be active year-round, but risk is highest during warmer months.
In general, Lyme disease transmission usually requires a tick to be attached for at least 24 hours, although other tick-borne illnesses may spread more quickly.
Because tick bites are often painless and easy to miss, regular checks after outdoor activity are essential.
How to Prevent Tick Bites
Simple prevention steps can significantly reduce your risk of Lyme disease:
- Use insect repellent with 20% DEET or EPA-approved ingredients
- Wear long sleeves and long pants when outdoors
- Avoid tall grass and stay in the center of trails
- Choose light-colored clothing to spot ticks more easily
- Check your child’s skin, scalp, and clothing after outdoor activities
- Shower within two hours of coming indoors
- Place clothes in the dryer on high heat after outdoor exposure
- Remove ticks promptly with fine-tipped tweezers

These small habits can help protect both children and adults during peak tick season.
When Should You Get Checked?
You should consider medical evaluation if your child or family member has:
- A rash after outdoor exposure
- Flu-like symptoms during tick season
- Unexplained fatigue or joint pain
- A known or suspected tick bite
Even if symptoms seem mild, early evaluation can help guide next steps and prevent complications.
Lyme Disease Care in Loudoun County and Northern Virginia
At Night Watch Urgent Care, we evaluate tick bites, rashes, and symptoms of Lyme disease with same-day care across Northern Virginia.
Our providers understand that early symptoms can be subtle, and we’re here to help you determine whether further evaluation or treatment is needed.
We’re open evenings and weekends, so you don’t have to wait to get your child checked.
CATEGORY
2/22/2026
POSTED
One of the most common questions healthcare providers hear is:
“How often should I actually get tested for STIs?”
The answer isn’t one-size-fits-all but it is simpler than most people expect.
At Night Watch Urgent Care in Aldie, many adults come in for STI testing not because something feels wrong, but because they want reassurance, responsibility, and clarity. Regular testing is a normal part of preventive healthcare, especially when life, relationships, or routines change.
This guide explains how often to test, why timing matters, and how same-day results make testing easier for busy Aldie residents.
The Simple Rule: Yearly or After a New Partner
For most sexually active adults, medical guidelines recommend STI testing at least once a year.
However, testing is also strongly recommended:
- After a new sexual partner
- Between partners
- If you or your partner have multiple partners
- If a partner tests positive
- If you’ve had unprotected sex, even once
Many STIs do not cause immediate symptoms. Testing based on time and exposure, not symptom, is what protects long-term health.
Why Waiting for Symptoms Isn’t Enough
A common misconception is that STI testing is only necessary when something feels wrong. In reality, most common STIs are often silent, especially early on.
- Chlamydia and gonorrhea frequently cause no symptoms
- Syphilis may cause a painless sore that’s easy to miss
- Early HIV infection can feel like a mild flu — or nothing at all
By the time symptoms appear, complications may already be developing. Regular testing catches infections early, when treatment is simplest and outcomes are best.
How Relationship Changes Affect Testing Frequency
Testing frequency should adjust with your life — not just your age.
You should consider testing more often than once a year if you:
- Have a new partner
- Are dating or using apps
- Are in an open or non-monogamous relationship
- Travel frequently for work or leisure
- Want reassurance before stopping condom use with a partner
Healthcare providers often recommend testing every 3–6 months for individuals with higher exposure risk.

Why Aldie Adults Choose Same-Day STI Testing
Traditional lab testing often means waiting several days, sometimes a full week for results. For many people, that waiting period causes unnecessary stress. Rapid STI testing provides same-day answers, often within minutes.
Many Aldie patients test during evenings or weekends, fitting care into real life — not the other way around.
What Testing Looks Like (and What It Doesn’t)
STI testing is usually quick and straightforward:
- Urine sample or swab for chlamydia and gonorrhea
- Finger-prick blood test for HIV and syphilis
- Results available the same visit in many cases
Testing does not require:
- Symptoms
- An exam unless medically indicated
- Explaining your personal life in detail
Confidentiality is protected under Virginia law, and care is provided without judgment.
Making STI Testing Part of Routine Healthcare
STI testing doesn’t have to be reactive. Many Aldie adults now treat it like:
- Annual physicals
- Dental cleanings
- Routine blood work
It’s a normal, responsible step, especially for people who value their long-term health and their partners’ wellbeing.
If you’re due for yearly testing, have a new partner, or just want peace of mind, same-day STI testing is available locally.
CATEGORY
2/06/2026
POSTED
easles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
At Night Watch Urgent Care, our pediatric team is hearing the same questions from families every day:
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
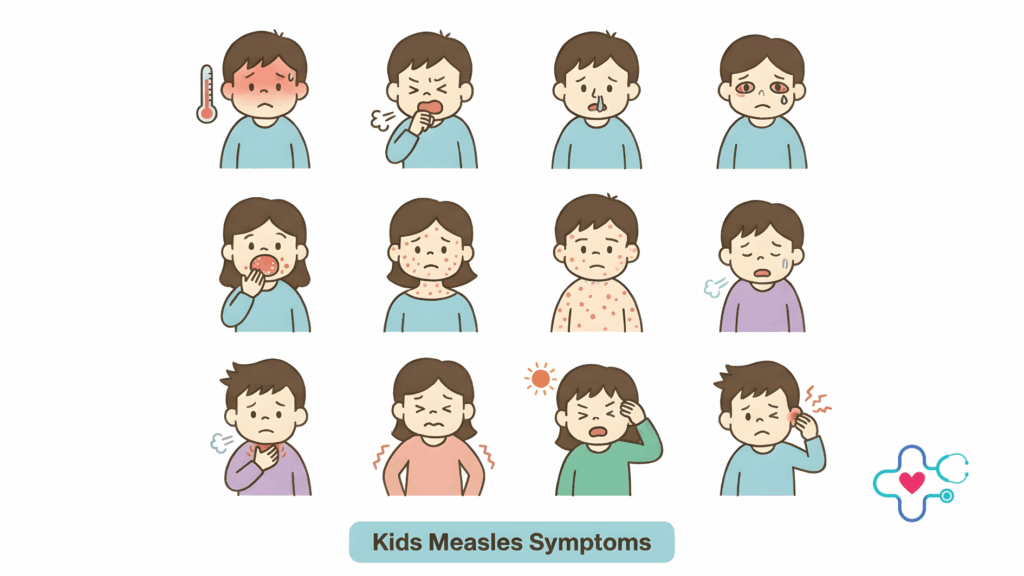
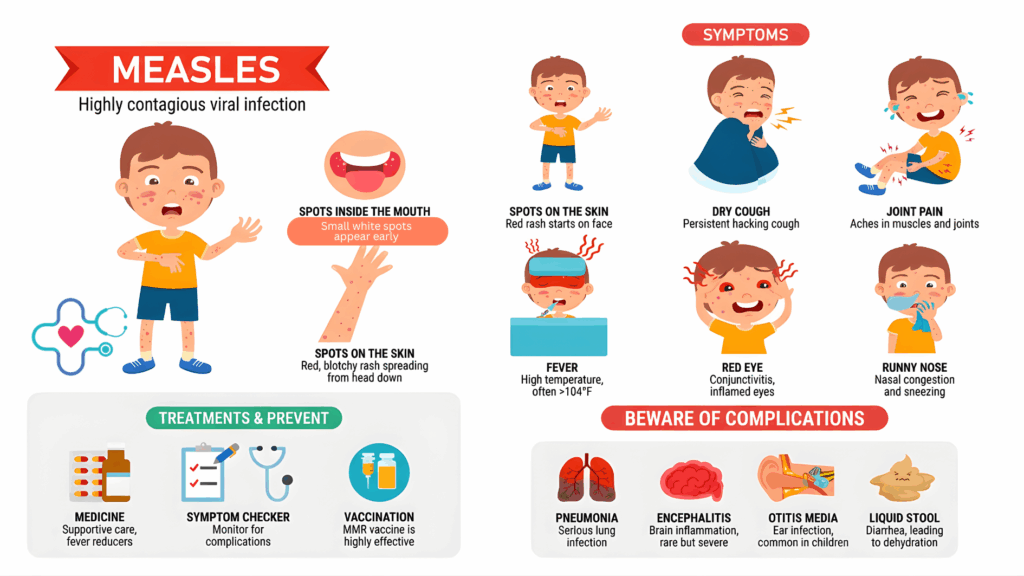
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
Families looking for measles care in Stone Ridge can rely on Night Watch Urgent Care for pediatric-focused evaluation and guidance.
Our Stone Ridge location offers evening and weekend hours, making it easier for parents to seek care when pediatric offices are closed. Our team focuses on careful assessment, clear communication, and helping families understand next steps.