blog spot
THE
health hub
A collection of helpful articles & information to spread awareness through education from our staff to you
CATEGORY
2/22/2026
POSTED
One of the most common questions healthcare providers hear is:
“How often should I actually get tested for STIs?”
The answer isn’t one-size-fits-all but it is simpler than most people expect.
At Night Watch Urgent Care in Aldie, many adults come in for STI testing not because something feels wrong, but because they want reassurance, responsibility, and clarity. Regular testing is a normal part of preventive healthcare, especially when life, relationships, or routines change.
This guide explains how often to test, why timing matters, and how same-day results make testing easier for busy Aldie residents.
The Simple Rule: Yearly or After a New Partner
For most sexually active adults, medical guidelines recommend STI testing at least once a year.
However, testing is also strongly recommended:
- After a new sexual partner
- Between partners
- If you or your partner have multiple partners
- If a partner tests positive
- If you’ve had unprotected sex, even once
Many STIs do not cause immediate symptoms. Testing based on time and exposure, not symptom, is what protects long-term health.
Why Waiting for Symptoms Isn’t Enough
A common misconception is that STI testing is only necessary when something feels wrong. In reality, most common STIs are often silent, especially early on.
- Chlamydia and gonorrhea frequently cause no symptoms
- Syphilis may cause a painless sore that’s easy to miss
- Early HIV infection can feel like a mild flu — or nothing at all
By the time symptoms appear, complications may already be developing. Regular testing catches infections early, when treatment is simplest and outcomes are best.
How Relationship Changes Affect Testing Frequency
Testing frequency should adjust with your life — not just your age.
You should consider testing more often than once a year if you:
- Have a new partner
- Are dating or using apps
- Are in an open or non-monogamous relationship
- Travel frequently for work or leisure
- Want reassurance before stopping condom use with a partner
Healthcare providers often recommend testing every 3–6 months for individuals with higher exposure risk.

Why Aldie Adults Choose Same-Day STI Testing
Traditional lab testing often means waiting several days, sometimes a full week for results. For many people, that waiting period causes unnecessary stress. Rapid STI testing provides same-day answers, often within minutes.
Many Aldie patients test during evenings or weekends, fitting care into real life — not the other way around.
What Testing Looks Like (and What It Doesn’t)
STI testing is usually quick and straightforward:
- Urine sample or swab for chlamydia and gonorrhea
- Finger-prick blood test for HIV and syphilis
- Results available the same visit in many cases
Testing does not require:
- Symptoms
- An exam unless medically indicated
- Explaining your personal life in detail
Confidentiality is protected under Virginia law, and care is provided without judgment.
Making STI Testing Part of Routine Healthcare
STI testing doesn’t have to be reactive. Many Aldie adults now treat it like:
- Annual physicals
- Dental cleanings
- Routine blood work
It’s a normal, responsible step, especially for people who value their long-term health and their partners’ wellbeing.
If you’re due for yearly testing, have a new partner, or just want peace of mind, same-day STI testing is available locally.
CATEGORY
2/16/2026
POSTED
Life in Aldie moves fast. Between work schedules, travel, relationships, and social plans, health concerns often get pushed to the bottom of the list—especially when nothing feels wrong.
But when it comes to sexually transmitted infections (STIs), feeling fine doesn’t always mean being fine.
In fact, studies show that up to 80% of common STIs cause no symptoms in their early stages, particularly infections like chlamydia and gonorrhea. These “silent” infections can spread quietly and lead to long-term health issues if left untreated.
At Night Watch Urgent Care in Aldie, adults walk in every week for discreet, rapid STI testing—not because they feel sick, but because they want clarity, peace of mind, and prevention.
This guide explains why silent STIs are common in Northern Virginia, how rapid testing works, and when it makes sense to get checked.
The Silent Spread in Aldie and Northern Virginia
Virginia continues to report high chlamydia rates—approximately 480 cases per 100,000 residents, with the highest concentration among adults aged 18–34. That age group makes up a significant portion of Aldie’s growing population of young professionals and couples.
Social gatherings, work travel, dating apps, and busy lifestyles all increase exposure risk—even for people who consider themselves careful.
One of the biggest misconceptions about STIs is that they always come with obvious warning signs. In reality:
- Up to 90% of chlamydia and gonorrhea cases begin without symptoms
- Early syphilis may cause a painless sore that’s easy to miss
- HIV can feel like a mild flu—or nothing at all—in early stages
Without testing, infections can persist for months or years.
Why “No Symptoms” Doesn’t Mean “No Risk”
When untreated, silent STIs can cause serious complications over time.
For women, risks include:
- Pelvic inflammatory disease (PID)
- Chronic pelvic pain
- Tubal scarring and infertility
- Increased risk during pregnancy
For men, complications may include:
- Epididymitis
- Prostate inflammation
- Fertility issues
Untreated syphilis can eventually affect the heart, brain, and nervous system, sometimes years after the initial infection.
At Night Watch Urgent Care, providers regularly see patients who had no symptoms but tested positive during routine screening—and were able to receive treatment immediately.
Real Aldie scenario:
A 29-year-old professional returned from a work trip feeling fine. No symptoms. A rapid test revealed chlamydia. Treatment was started the same visit, preventing long-term complications and further spread.
Why Symptoms Can Mislead — and Testing Doesn’t
STIs don’t spread only through penetrative sex. Oral, anal, and skin-to-skin contact can transmit infections, and while condoms significantly reduce risk, they don’t eliminate it—especially for herpes, HPV, and syphilis.
The most common silent infections include:
- Chlamydia: The leading preventable cause of infertility in young adults
- Gonorrhea: Often symptom-free, especially in women
- Syphilis: Early signs are subtle but consequences can be severe
Medical guidelines recommend:
- Annual STI testing for sexually active adults
- Every 3–6 months for those with new or multiple partners
Testing is about prevention—not judgment.
Rapid STI Testing at Night Watch Urgent Care Aldie
Traditional lab testing often means waiting days for results. At Night Watch Urgent Care in Aldie, rapid STI testing delivers answers the same visit.
What to Expect
| Test | Sample | Results | Availability |
| Chlamydia / Gonorrhea | Urine or swab | 15–30 minutes | Walk-in daily |
| Syphilis / HIV | Finger-prick blood | ~20 minutes | Same visit |
| Full STI Panel | Combination | Same day | Evenings & weekends |
- Lab-level accuracy (≈97%)
- Fully confidential under Virginia privacy laws
- Insurance accepted; affordable self-pay options available
- Treatment often started immediately if positive
Most tests involve either a urine sample or a quick swab—no invasive procedures.
Why Aldie Adults Choose to Test Early
In Northern Virginia, providers frequently see STI-related issues disguised as other concerns:
- Recurrent UTIs
- Pelvic discomfort
- Joint pain
- Fatigue
- Fertility struggles
Another real case:
A patient returned from vacation with mild pelvic discomfort. Rapid testing revealed gonorrhea—caught early and treated the same day.
Infertility remains one of the most preventable consequences of untreated chlamydia. Early detection makes all the difference.

If you’ve been wondering whether testing makes sense, it probably does. We’re open evenings and weekends when most offices are closed. Walk-ins welcome.
CATEGORY
2/06/2026
POSTED
easles is appearing in more communities across the U.S., and many parents are understandably concerned. While measles may feel like an illness from the past, it remains one of the most contagious viral infections affecting children today — and it often begins in a way that’s easy to miss.
At Night Watch Urgent Care, our pediatric team is hearing the same questions from families every day:
How does measles start? How worried should I be? And when should I bring my child in?
This guide is designed to give parents clear, practical information so you can recognize symptoms early, understand how measles spreads, and feel confident about next steps if your child becomes ill.
What Is Measles and Why Is It So Contagious?
Measles is a viral illness that spreads through the air when an infected person coughs, sneezes, or breathes. Unlike many other childhood viruses, measles does not require close contact to spread.
The virus can remain in the air for up to two hours after an infected person leaves a room, meaning exposure can occur in classrooms, daycare centers, grocery stores, or medical offices without direct interaction.
What makes measles especially challenging is that children are contagious before parents realize it’s measles. By the time the classic rash appears, the virus may have already spread to others.
This is why early recognition and prevention play such an important role in protecting families and communities.
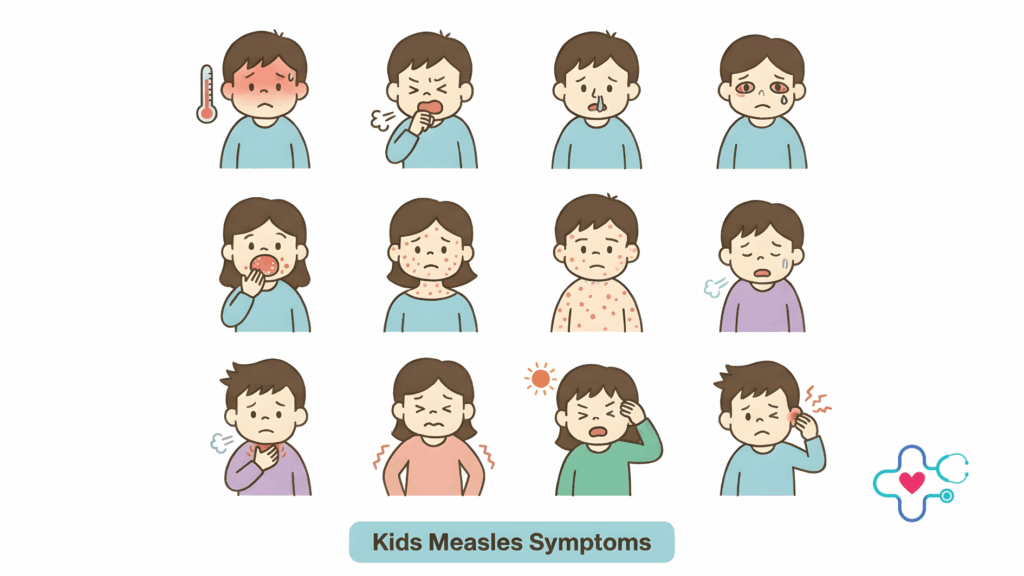
Early Measles Symptoms Parents Often Miss
Many parents associate measles with a rash — but the rash comes later.
In the early stage, measles often looks like a severe cold or flu. Symptoms may include:
- High fever, often rising quickly
- Cough
- Runny nose
- Red, watery, or irritated eyes
- Fatigue, irritability, or decreased appetite
Because these symptoms are common with many viral illnesses, measles can be difficult to identify at first. A key difference parents often notice is how sick their child looks and feels, especially when fever is high and persistent.
When the Rash Appears
The measles rash typically develops three to five days after fever begins. It usually:
- Starts on the face or hairline
- Spreads downward to the neck, trunk, arms, and legs
- Appears as flat red spots that may merge together
If your child develops fever followed by a spreading rash, or symptoms seem to worsen instead of improve, it’s important to contact a medical provider.
Why Measles Can Be Serious for Children
While many children recover from measles, it is not always a mild illness. Some children are at higher risk for complications, including:
- Infants under 12 months
- Children who are not fully vaccinated
- Children with asthma or chronic medical conditions
- Pregnant individuals and immunocompromised family members
Complications can include ear infections, dehydration, pneumonia, and in rare cases, serious neurologic issues. This is why prompt guidance and careful monitoring are important, even if symptoms seem manageable at first.
How Parents Can Protect Their Children From Measles
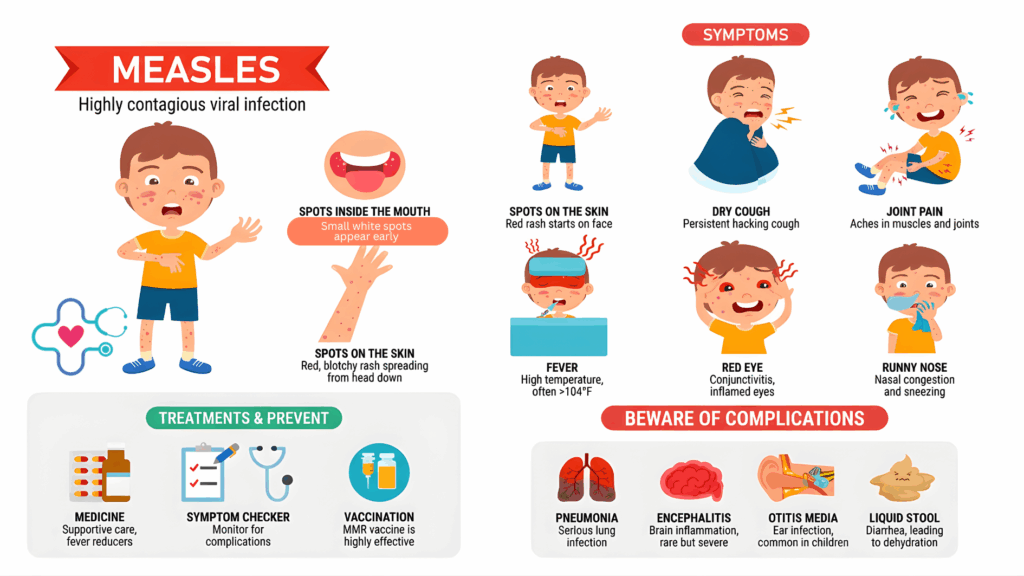
MMR Vaccination
The MMR (measles, mumps, rubella) vaccine is the most effective way to prevent measles. Two doses provide strong, long-lasting protection and significantly reduce the risk of severe illness and complications.
If you’re unsure whether your child is up to date on vaccinations or have questions about timing, a pediatric provider can help review your child’s immunization history and answer concerns.
Reducing Exposure
During times of increased measles activity:
- Avoid close contact with anyone who has fever and rash symptoms
- Be cautious in crowded indoor settings when possible
- Notify your healthcare provider if your child may have been exposed
Protecting High-Risk Family Members
If your household includes infants, pregnant individuals, or people with weakened immune systems, extra care is important. Keeping eligible family members vaccinated and limiting exposure to illness helps protect those most vulnerable.
When to Call Before Coming In
Because measles spreads so easily, calling ahead before visiting urgent care is essential.
Please contact a medical provider first if your child has:
- Fever along with a rash
- Known exposure to someone with measles
- Symptoms and is not fully vaccinated
Calling ahead allows our team to prepare appropriately and helps protect other children and families in our care.
Seek urgent or emergency care immediately if your child experiences:
- Trouble breathing or fast, labored breathing
- Extreme sleepiness, confusion, or difficulty staying awake
- Signs of dehydration such as very dry mouth, no tears, or minimal urination
- A very high fever that does not respond to medication
You never have to make these decisions alone. We are always here to help guide you.
Families looking for measles care in Stone Ridge can rely on Night Watch Urgent Care for pediatric-focused evaluation and guidance.
Our Stone Ridge location offers evening and weekend hours, making it easier for parents to seek care when pediatric offices are closed. Our team focuses on careful assessment, clear communication, and helping families understand next steps.
CATEGORY
1/31/2026
POSTED
Famous Last Words Before Someone Ends Up at Urgent Care
The scene: Sunday dinner. The whole family’s cooking together. It’s going to be so fun.
One hour later:
- 🔥 Someone grabbed a hot pan handle without a mitt
- 🔪 Your teenager “didn’t realize the knife was that sharp”
- 💦 Your 8-year-old spilled boiling water on their hand
- 🩹 You’re frantically Googling “how bad does a cut have to be for stitches”
Welcome to family cooking. It’s a contact sport.
🔥 The Kitchen Injury Hall of Fame
Here’s what we see constantly at Night Watch:
1. Burns (The Most Common)
🔥 Hot pan handles
“I forgot it was still hot.” Classic. Second-degree burns from cast iron, stainless steel, or oven pans.
💧 Boiling water/oil splatter
Pasta water boils over. Bacon grease splatters. Someone bumps the pot. Instant burn.
🔥 Oven doors
Reaching in to grab something, arm grazes the oven rack or door. Burns in stripes.
🍲 Steam burns
Opening a pot lid the wrong way. Steam escapes directly onto hand/face. Worse than you’d think.
2. Cuts (The Bloody Ones)
🔪 Knife slips
Chopping onions, knife slips, finger gets sliced. Happens in a split second.
🥫 Can opener injuries
Sharp lid edges. Manual can openers. Deep cuts on fingers or palms.
🍷 Broken glass
Wine glass shatters in sink. Cutting board slides, glass falls. Lacerations on hands.
🥔 Mandoline/grater accidents
“I thought I was being careful.” Mandoline slicers are ER visit magnets. Deep cuts, fingertip injuries.
3. Other Kitchen Mishaps
- 🧊 Slipping on spills (oil, water, dropped food)
- 🫰 Smashed fingers (cabinet doors, drawers, dropped pots)
- 🔥 Grease fires (someone adds water—don’t do that)
- ☠️ Food poisoning (undercooked meat, cross-contamination)
Burns: When to Come In
First-Degree Burns (Superficial)
What it looks like: Red skin, painful, no blisters. Like a bad sunburn.
Treatment: Cool water, aloe, pain relief. Usually can treat at home.
Second-Degree Burns (Partial Thickness)
What it looks like: Red, very painful, BLISTERS forming.
When to come in:
- Larger than 3 inches
- On face, hands, feet, joints, or genitals
- Blisters are large or popping
- Signs of infection developing
Third-Degree Burns (Full Thickness)
What it looks like: White, charred, or leathery skin. May not hurt (nerves damaged).
Action: CALL 911. This needs emergency care.
🔪 Cuts: When You Need Stitches
Come to Night Watch if:
- Bleeding doesn’t stop after 10 minutes of pressure
- Cut is deep (you can see fat, muscle, or bone)
- Edges gape open when you release pressure
- On face, hand, or over a joint
- Numbness, tingling, or inability to move fingers/hand
- Caused by dirty or rusty object
- Happened more than 6-8 hours ago
Time matters. Cuts heal best when closed within 6-8 hours.
What We Do at Night Watch
For Burns:
- Clean and assess burn depth
- Proper wound care (special dressings)
- Pain management
- Antibiotics if needed
- Tetanus booster if due
For Cuts:
- Stop bleeding and clean wound
- Assess for nerve/tendon damage
- Stitches, skin glue, or steri-strips
- Tetanus shot if needed
- Follow-up care instructions
🛡️ Preventing Kitchen Disasters
For Burns:
- ALWAYS use oven mitts or towels
- Turn pot handles inward (away from edge)
- Lift pot lids away from you (steam escapes backward)
- Keep kids away from stove/oven when in use
- Don’t wear loose sleeves near open flames
For Cuts:
- Keep knives sharp (dull knives slip more)
- Cut AWAY from your body
- Use cutting boards (stable surface)
- Pay attention (no phone while chopping)
- Store knives safely (not loose in drawers)
Supervising Kids in the Kitchen
Age-appropriate tasks:
Ages 3-5: Washing vegetables, mixing (cold ingredients), setting table
Ages 6-8: Measuring, pouring, stirring, using butter knives
Ages 9-12: Using sharp knives WITH SUPERVISION, basic stove use
Teens: Can handle most tasks but still need supervision with hot oil, deep frying
🍳 Family cooking: fun until someone needs stitches.
We’ll patch you up and get you back to dinner.
CATEGORY
1/29/2026
POSTED
Your teenager: “My head hurts.”
Your 8-year-old: “My eyes feel weird.”
You: *currently rubbing your temples while reading this on your phone*
What’s going on?
Let’s do the math on your family’s screen time:
📊 The Screen Time Tally
Average American household:
- Adults: 11+ hours per day on screens (work + personal)
- Teens: 7-9 hours per day (school Chromebooks + phones + gaming)
- Kids (8-12): 4-6 hours per day (tablets + school devices + TV)
That’s more waking hours looking at screens than NOT looking at screens.
And your eyes? They’re tired.
What’s Actually Happening to Your 👁️
Digital Eye Strain (Computer Vision Syndrome) is real. And it affects everyone in your house.
What causes it:
1. Reduced Blinking
Normal blink rate: 15-20 times per minute | Screen blink rate: 5-7 times per minute
Result: Dry, irritated eyes
2. Blue Light Exposure
Screens emit high-energy blue light that your eyes have to work harder to focus. Can disrupt sleep patterns too.
3. Close-Up Focus
Your eye muscles strain to maintain focus at close range for hours. They’re literally working overtime.
4. Poor Posture
Hunching over devices = neck strain = tension headaches
🤕 The Symptoms Everyone’s Experiencing
- 💧 Dry, irritated eyes
- 😵 Headaches (especially forehead/temples)
- 🌫️ Blurry vision
- 😫 Eye fatigue
- 💢 Neck and shoulder pain
- 😴 Difficulty focusing
- ☀️ Light sensitivity
Sound familiar? Yeah. That’s everyone in your house right now.
The 20-20-20 Rule (Actually Works)
Every 20 minutes, look at something 20 feet away for 20 seconds.
Sounds simple. Nobody does it. But it genuinely helps.
Why it works: Gives your eye muscles a break from constant close-up focus. Allows them to relax.
How to remember: Set phone reminders, use apps like “Eye Care 20 20 20,” stick Post-it notes on monitors.
Other Things That Help
- Adjust screen brightness – match it to room lighting
- Use blue light filters – most devices have built-in “night mode”
- Position screens properly – 20-26 inches away, slightly below eye level
- Increase text size – stop squinting
- Use artificial tears – combat dryness
- Blink intentionally – sounds weird, but your eyes forget to
- Take actual breaks – walk away from screens regularly
When Screen Time Headaches Aren’t Just Screen Time
Come to Night Watch if:
- Headaches are severe or getting worse
- Vision changes persist after screen breaks
- You see halos, double vision, or flashing lights
- Eye pain (not just strain)
- Red, swollen, or irritated eyes that don’t improve
- Headaches with nausea, vomiting, or fever
These could indicate migraines, eye infections, vision problems, or other conditions that need evaluation.
Do You Need 👓 ?
Sometimes “digital eye strain” is actually undiagnosed vision problems.
Signs you might need an eye exam:
- Frequent headaches when reading or using screens
- Squinting to see clearly
- Sitting very close to screens
- Blurry vision that doesn’t clear with breaks
We can evaluate and refer to an optometrist if needed.
Kids & Screen Time
Children’s eyes are still developing. Excessive screen time can affect:
- Vision development
- Eye focusing abilities
- Sleep patterns (blue light disruption)
- Risk of myopia (nearsightedness)
AAP recommendations:
- Under 2: Avoid screens (except video chatting)
- Ages 2-5: 1 hour/day of quality programming
- Ages 6+: Consistent limits, not interfering with sleep/activity
📱 Everyone’s head hurts. Everyone’s eyes are tired.
We can help figure out if it’s just screens – or something more.
CATEGORY
1/22/2026
POSTED
How Many Times Can One Kid Get Sick in Three Months?
October: Strep throat.
November: Cold #1. Then cold #2. Then stomach bug.
December: Flu. Another cold. Pink eye from their sibling.
January: You’ve lost count.
At this point, you’re Googling “is it possible for a child to have a broken immune system” at 2 AM while they cough in the next room.
Deep breath. Let’s talk about this.
The Numbers (That Will Make You Feel Better)
Here’s what’s actually normal for kids:
Ages 0-2 Years
6-12 illnesses per year (sometimes more if in daycare)
Ages 3-5 Years
8-12 illnesses per year (peak sick years)
School-Age Kids
5-8 illnesses per year (finally calming down)
So when you feel like your kid is ALWAYS sick? They kind of are. And that’s… normal.
🦠 “But Why Is It CONSTANT?”
Let’s do the math:
- Average cold lasts 7-10 days
- Kids get 6-12 colds per year
- That’s 42-120 days of being sick
- Plus stomach bugs, ear infections, strep, flu…
They’re literally sick for 1/3 of the year.
You’re not imagining it. They are always sick.
🏫 The Daycare/School Effect
Kids in daycare or school get sick significantly more than kids at home.
Why?
- Close contact with other kids (who are also germ factories)
- Shared toys, books, tablets
- Kids touch EVERYTHING then put hands in mouth
- Indoor air circulation spreads respiratory viruses
- 200+ cold viruses circulating at any given time
First year of daycare/preschool? Buckle up. It’s going to be a ride.
💪 Their Immune System Is Working
Here’s the good news: Every single illness is training their immune system.
Think of it like this:
→ Each virus they catch = their body learns how to fight it
→ Next time they encounter that virus = faster, stronger response
→ By age 5-6 = built immunity to most common childhood viruses
It’s not a broken immune system. It’s an immune system at boot camp.
When to Actually Worry
Most recurrent illness is normal. But here’s when it’s NOT:
- Infections that don’t respond to treatment
- Multiple serious infections per year (pneumonia, meningitis, bloodstream infections)
- Recurrent abscesses or deep skin infections
- Failure to thrive or poor weight gain
- Family history of immune deficiency disorders
- Chronic diarrhea or thrush
Common colds, stomach bugs, and ear infections? Normal. Pneumonia three times in six months? Not normal.
How We Help at Night Watch
When your kid gets sick (again), we can:
- Diagnose what they have (strep, flu, RSV, COVID, ear infection, etc.)
- Provide treatment to help them recover faster
- Evaluate their pattern of illness and determine if testing is needed
- Refer to specialists if immune testing is warranted
- Reassure you that yes, this is probably normal
📝 Keeping Track
If you’re worried, keep a simple log:
- Date of illness
- Type (cold, stomach bug, ear infection, etc.)
- Treatment given
- How long it lasted
Bring it to your visit. It helps us see patterns.
Sick again? Yeah, we know. It’s exhausting. But their immune system is probably fine. Promise.
CATEGORY
1/20/2026
POSTED
Now Half the School Has Pink Eye.
Monday morning. One kid shows up to school with goopy, red eyes.
By Wednesday? Five more cases.
By Friday? The classroom looks like a zombie movie.
Welcome to pink eye season.
🦠 Why Pink Eye Spreads Like Wildfire
Pink eye (conjunctivitis) is insanely contagious. Here’s why:
- Kids touch everything – desks, toys, doorknobs, each other
- They rub their eyes constantly – spreading infected discharge on their hands
- They share stuff – pencils, water bottles, tablets, face paint
- Viral pink eye can live on surfaces for hours to days
- Symptoms can take 1-3 days to appear – they’re contagious before they look sick
One infected kid touches a keyboard. Another kid touches the same keyboard. Rubs their eye. Boom. Pink eye.
👀 What Pink Eye Actually Looks Like
Classic symptoms:
- 👁️ Red or pink appearance in the white of the eye
- 💧 Watery discharge (viral) or thick, goopy discharge (bacterial)
- 😫 Eyes crusted shut in the morning
- 😖 Itchy, gritty feeling
- 💦 Excessive tearing
- ☀️ Sensitivity to light
The Three Types of Pink Eye
1. Viral Pink Eye
Caused by:
Same viruses that cause colds. Often accompanies upper respiratory infections.
How to spot it:
- Watery, clear discharge
- Extremely itchy
- Usually starts in one eye, spreads to the other
- May have cold symptoms too
Treatment:
No antibiotics needed (it’s a virus). Runs its course in 7-14 days. We provide supportive care and rule out bacterial infection.
2. Bacterial Pink Eye
How to spot it:
- Thick, yellow or green discharge
- Eyes glued shut with crusty goop
- More pain than viral
- Can affect one or both eyes
Treatment:
Antibiotic eye drops. Usually clears up in 3-5 days with treatment.
3. Allergic Pink Eye
How to spot it:
- Both eyes affected at the same time
- Very itchy
- Watery discharge
- Other allergy symptoms (sneezing, runny nose)
Treatment:
Antihistamine eye drops, avoid allergens. Not contagious.
When to Come to Night Watch
Come in if:
- Eyes are red and goopy
- You need a school/work note (most require medical clearance)
- Thick, colored discharge (likely bacterial = needs antibiotics)
- Pain or vision changes
- Symptoms not improving after 3-4 days
- Child under 1 year old with pink eye
🧼 Stop the Spread
Pink eye is preventable. Here’s how to protect your family:
- Wash hands constantly – especially after touching eyes
- Don’t touch or rub eyes
- Don’t share towels, pillows, or makeup
- Change pillowcases daily during infection
- Disinfect surfaces – doorknobs, tablets, keyboards, phones
- Keep infected kids home until cleared by doctor
- Throw out old eye makeup after pink eye
What We Do at Night Watch
- Examine eyes to determine type of pink eye
- Prescribe antibiotic drops if bacterial
- Provide symptom relief recommendations
- Write school/work clearance notes
- Educate on preventing spread to family members
⏰ When Can They Go Back?
Bacterial pink eye: 24 hours after starting antibiotic drops
Viral pink eye: When discharge is gone and eyes are no longer red
Allergic pink eye: Can return immediately (not contagious)
👁️ Pink eye spreads fast. Treatment is easy. Get it diagnosed. Get it treated. Get back to life.
CATEGORY
1/16/2026
POSTED
Now Your Kid Can’t Stop Coughing.
January in Virginia. The heat’s cranked up. The air is bone dry. Your kid wakes up with a bloody nose, dry throat, irritated skin.
So you do what every good parent does: You buy a humidifier.
You set it up in their room. You run it every night. Problem solved, right?
Except now they’re coughing more. They’re wheezing. They say their chest feels tight.
Plot twist: The thing you bought to help them breathe better is making them sick.
🦠 How Humidifiers Become Germ Factories
Here’s what’s happening inside that humidifier:
Water sits in the tank. Even for a day or two. Room temperature. Dark. Perfect breeding ground for bacteria and mold.
The humidifier aerosolizes that water. It turns it into a fine mist and sprays it into the air your child breathes.
Your child inhales bacteria and mold spores all night long.
Congratulations. You just turned your kid’s bedroom into a petri dish with a fan.
“Humidifier Fever” Is Real
It’s called “humidifier fever” or “humidifier lung,” and it’s more common than you think.
Symptoms include:
- Persistent cough (especially at night)
- Wheezing or difficulty breathing
- Chest tightness
- Fever and chills
- Fatigue
- Flu-like symptoms that won’t go away
The kicker? Symptoms often get worse at night (when the humidifier is running) and improve during the day (when they’re at school).
🔬 What’s Growing in There?
Studies have found these delightful things in dirty humidifiers:
Bacteria
Legionella (yes, the Legionnaires’ disease bacteria), Pseudomonas, and other respiratory pathogens. Can cause serious lung infections.
Mold & Fungi
Black mold, Aspergillus, and other fungi. Trigger allergies, asthma attacks, and respiratory infections.
Mineral Dust (“White Dust”)
From tap water. Fine particles settle on furniture AND get inhaled into lungs. Can cause respiratory irritation.
When to Come to Night Watch
Bring your child in if they have:
- Persistent cough that gets worse at night
- Wheezing or difficulty breathing
- Chest pain or tightness
- Fever with respiratory symptoms
- Symptoms that improve away from home
- Asthma that’s suddenly worse
We can evaluate for respiratory infections, provide breathing treatments, and help you figure out if environmental factors (like your humidifier) are making them sick.
🧼 How to Clean Your Humidifier (Properly)
Most people don’t clean their humidifiers nearly enough.
Here’s what you should actually be doing:
- Daily: Empty tank, rinse with fresh water, refill
- Every 3 days: Deep clean with white vinegar (removes mineral buildup)
- Weekly: Disinfect with 3% hydrogen peroxide or bleach solution
- Always: Use distilled or demineralized water (not tap water)
- Replace filters: According to manufacturer instructions
⚠️ Red Flags Your Humidifier Is Dirty
- Visible slime or film in the tank
- Musty or moldy smell
- White dust on furniture near humidifier
- Mineral buildup (crusty deposits)
- Can’t remember when you last cleaned it
If you see any of these? Stop using it immediately and deep clean.
Better Options
- Warm mist humidifiers: Boil water, killing bacteria before releasing steam
- UV light humidifiers: Kill microorganisms before misting
- Easier alternatives: Bowl of water near heat vent, wet towels, more houseplants
- Keep humidity 30-50%: Too high = mold growth in your home
Your humidifier should help your child breathe. Not turn their bedroom into a science experiment.
CATEGORY
1/12/2026
POSTED
(And Your New Patient at Night Watch)
Christmas morning. The kids unwrap the last present. Inside the crate: one adorable, wiggly, 8-week-old puppy.
Everyone screams with joy. The puppy is thrilled. Maybe a little too thrilled.
Fast forward three days: Your 7-year-old has scratches down both arms. Your teenager has a puncture wound on their hand. You have a bite mark that’s starting to look… concerning.
Welcome to new pet ownership.
🐕 Why Puppies (and Kittens) Bite
First, let’s be clear: Your new puppy isn’t aggressive. They’re just being a puppy.
Puppies explore the world with their mouths. They play-bite. They nip. They chew on literally everything—including your fingers, your toes, your kid’s hair.
Kittens? Even worse. Those tiny needle-sharp claws and teeth can do serious damage, especially when they’re playing or scared.
The problem? Their mouths are full of bacteria. And those cute little teeth can break skin surprisingly easily.
🚨 When That Cute Bite Needs Medical Attention
Come to Night Watch if:
- The bite broke the skin (especially if it’s a puncture wound)
- It’s on the face, hand, or near a joint
- The wound is deep or won’t stop bleeding
- Signs of infection appear (redness, swelling, warmth, pus, red streaks)
- It happened more than 8 hours ago and wasn’t cleaned properly
- You’re not sure of the pet’s vaccination status (adopted from shelter, stray, etc.)
🐱 Cat Scratches: Small But Mighty Dangerous
Got a new kitten for the holidays? Those tiny scratches are not harmless.
Cat Scratch Disease (yes, it’s real): Caused by bacteria in cat saliva that gets on their claws. Can cause fever, swollen lymph nodes, fatigue, and in rare cases, more serious complications.
Watch for:
- Red, raised bump at scratch site (appears 3-14 days after)
- Swollen lymph nodes (especially under arms or in neck)
- Fever
- Fatigue or headache
Dog Bites: Not Just About Infection
Even your sweet, friendly new puppy can cause injury:
Puncture wounds:
Deep, narrow wounds that don’t bleed much but push bacteria deep into tissue. High infection risk.
Crushing injuries:
Even without breaking skin, dog bites can crush tissue, blood vessels, nerves. Can cause serious damage to hands especially.
Tearing:
Jagged wounds that may need stitches.
What We Do at Night Watch
When you come to Night Watch with an animal bite or scratch:
- Thorough wound cleaning (irrigation to remove bacteria)
- Evaluation for tissue damage (nerves, tendons, blood vessels)
- Stitches if needed (though some bites are left open to prevent infection)
- Antibiotics (especially for punctures, cat bites, hand/face wounds)
- Rabies evaluation (if vaccination status unknown)
Preventing Pet Injuries at 🏡
Tips for the first few weeks:
- Supervise all interactions with young children
- Teach kids not to put hands near puppy’s mouth during play
- Redirect biting to appropriate chew toys
- Trim kitten nails regularly
- Don’t use hands as toys (teaches them it’s okay to bite/scratch)
- Start training early (puppy classes, bite inhibition)
🩹 First Aid at Home
If your new pet bites or scratches someone:
- Wash immediately with soap and running water for 5+ minutes
- Apply pressure if bleeding
- Don’t seal puncture wounds with bandages – let them drain
- Then get it checked at Night Watch
New pets are adorable. Animal bites are not. Get it checked before it gets infected.
CATEGORY
1/09/2026
POSTED
When Your Teen’s January Exhaustion Isn’t Normal
January hits different when you’re a teenager.
Two weeks of sleeping in, staying up late, zero responsibilities. Then suddenly: 6:30 AM alarms, seven-hour school days, homework, activities, repeat.
Of course they’re exhausted. Right?
But you’re starting to wonder. Because it’s been three weeks, and they’re not adjusting. If anything, they’re getting worse.
🎒 The January Slump vs. Something More
Yes, getting back into the school routine is rough. And yes, teenagers need 8-10 hours of sleep (which most don’t get).
But here’s what’s NOT normal:
- Sleeping 12+ hours and still exhausted
- Falling asleep in class regularly
- Can’t stay awake even when they try
- Zero energy for things they used to love
- Getting worse as January goes on
- Other symptoms (sore throat, pale skin, weight changes)
If this sounds like your teen, it’s time to get them checked.
🩺 What Could Be Going On?
When exhaustion is this severe, there’s often a medical explanation:
😷 Mononucleosis (“Mono”)
The most common cause of extreme teen fatigue. Spread through saliva (shared drinks, kissing), mono causes weeks of crushing exhaustion, sore throat, and swollen lymph nodes. No amount of sleep helps until it runs its course.
🩸 Anemia
Low iron = not enough oxygen getting to tissues. Especially common in teenage girls due to menstruation. Symptoms include constant tiredness, pale skin, dizziness, and shortness of breath during normal activities.
Thyroid Problems
An underactive thyroid (hypothyroidism) slows your entire metabolism. Everything feels harder – waking up, concentrating, staying warm. Weight gain, dry skin, and “brain fog” are also common.
💤 Sleep Disorders
Sleep apnea, insomnia, restless leg syndrome – yes, teens get these too. They might be in bed for 10 hours, but not actually getting restorative sleep.
😔 Depression or Anxiety
Mental health struggles manifest physically. Depression especially causes overwhelming fatigue, loss of interest in activities, and difficulty getting out of bed – even after a full night’s sleep.
🍔 Nutritional Deficiencies
Vitamin D, B12, and other deficiencies cause serious fatigue. Common in teens who skip meals, eat mostly processed foods, or follow restrictive diets without proper supplementation.
🏥 How We Can Help
At Night Watch, we take teen exhaustion seriously. Here’s what we can do:
- Comprehensive blood work: Test for mono, anemia, thyroid function, vitamin levels
- Physical examination: Check for swollen lymph nodes, pale skin, other physical signs
- Rapid testing: Strep, flu, COVID if illness suspected
- Mental health screening: And referrals to appropriate providers
- Treatment or referral: Based on what we find
Most causes of extreme exhaustion are treatable – once you know what you’re dealing with.
📚 When School Performance Tanks
Here’s a major red flag: your formerly good student is suddenly struggling.
- Can’t concentrate in class
- Falling asleep during lectures
- Can’t complete homework
- Memory problems
- Grades dropping
This isn’t laziness or “senioritis.” Something is physically or mentally preventing them from functioning normally.
⏰ Don’t Wait
Bring them to Night Watch if:
- Exhaustion has lasted more than 2 weeks
- It’s affecting school or activities
- They’re sleeping 10+ hours and still tired
- Other symptoms are present
- Your parental instinct says something’s wrong
Sometimes “I’m just tired” means something’s really wrong. Let’s figure out what it is.